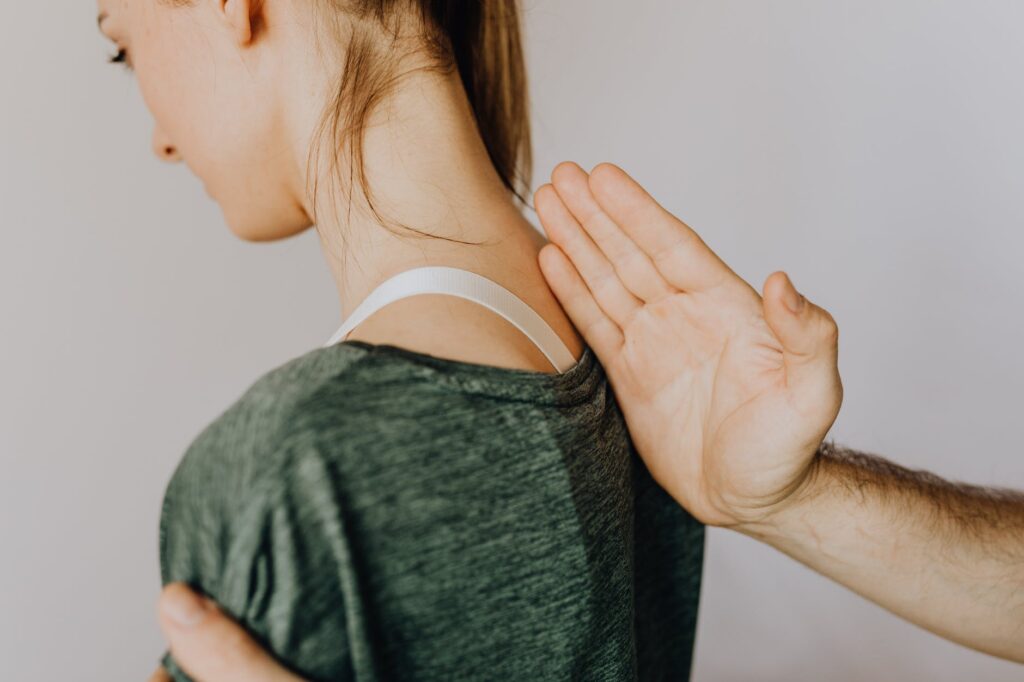
Few human injuries are as catastrophic as those to the spine. An accident, disease or act of violence affecting the spine can result in poor function – even paralysis – almost anywhere in the body.
The spinal column is enormously complex, with limited capacity for regeneration and any health implications are usually long-term and chronic.
While there is no known way to repair a spinal cord injury (SCI), scientists may be on the cusp of some important breakthroughs. New approaches are being taken to reverse the nerve damage, with some researchers attempting to reshape the architecture of the spinal cord using materials engineered in the laboratory.
Prof Paula Marques, material scientist at the University of Aveiro in Portugal and her colleagues, are seeking to mould a particular biomaterial into a scaffold that can replace damaged spinal tissue. This will create a working bridge over an injured area giving the brain an alternative pathway to communicate with the body.
The hope is that, within the next decade, these biomaterials will result in radical new treatments for the 250-500 000 people who suffer a spinal cord injury around the world every year.
‘Even a small improvement in treatment can lead to a big change to quality of life,’ said Prof Marques.
Nerve regeneration
In addition, the scaffold implant would support the regeneration of natural nerve cells, enabling the body eventually to resume its natural function unassisted.
Prof Marques is the principal researcher of the NeuroStimSpinal project, an EIC Pathfinder project under Horizon 2020 focusing on graphene-based material combined with a protein-rich material derived from humans known as a ‘decellularised extracellular matrix’. In the human body, an extracellular matrix provides the structure and support to living cells.
This blend of matrix and graphene-based material creates a 3D structure that skilfully mimics the morphology of the native spinal cord. It will form the backbone – as it were – of the project’s implant.
“
Even a small improvement in treatment can lead to a big change to quality of life Professor Paula Marques, NeuroStimSpinal
Graphene (a sheet of carbon atoms) shows excellent electrical properties, meaning a current can run along it – a prerequisite for any material that might be employed to send electrical impulses along the spinal cord.
Importantly, the scaffold is porous, meaning cells and spinal fluids can pass through it. It’s also biocompatible, preventing rejection by the body, and biodegradable, allowing it to be programmed to degrade over time.
Restoring function
Prof Marques describes her work as ‘disruptive’ and says the potential prize of restoring function to people with paralysis is huge.
‘I see real hope,’ she said. ‘My only frustration is that we can’t move forward faster with this research – spinal cord injury has such a big impact on human life.’
There are two main types of cells in nerve tissue: neurons, which transmit electrical impulses, and glial cells, which are non-conductive and provide a support system for the neurons.
In lab experiments, the NeuroStimSpinal team – which includes experts in material science, electronic engineering, physics and biology – have found that when their scaffold is seeded with embryonic neural progenitor cells (cells that renew themselves and have the potential to develop into either neuronal or glial cells) and an electrical stimulus is applied, the ‘blank’ stem cells successfully differentiate into a mixture of the two cell types.
‘This is very encouraging,’ said Prof Marques. ‘It shows that the scaffold can provide a good environment for nerve cell regrowth.’
Her group is one of just a handful around the world that has managed to make neural stem cells develop into new cell lineages in lab conditions.
However, to date, no such success has been achieved in live animals. Prof Marques wants her next round of experiments to set SCI research on a new course.
“
My only frustration is that we can’t move forward faster with this research – spinal cord injury has such a big impact on human life Professor Paula Marques, NeuroStimSpinal
In the months ahead, her team will transplant miniature versions of their scaffold into rats. An electric current will be applied to the implant through a control unit inserted under the animals’ skin to accelerate tissue regrowth. If these experiments show regeneration of the animals’ spinal cord is possible with the scaffold in place, Prof Marques will apply for fresh funding to take her work to the next level.
‘I hope we can contribute with our scientific knowledge to take a step forward towards SCI repair,’ she said.
Catastrophic stroke
A stroke is another catastrophic life event that can result in damage to the nervous system. Strokes, besides being the number two cause of death worldwide, are the third-leading cause of disability-adjusted life years (DALY), a metric used to assess the burden of death and disease.
Scientists have yet to find a way to replace the dead brain cells that result from a clot blocking the flow of blood and oxygen to the brain, but they are starting to exploit the latest technology – such as advances in virtual reality (VR) – to help patients recover from some of the long-term consequences.
After a stroke, hands can become stiff due to disrupted connections between the brain and the hand muscles. This “spasticity” can make it hard, almost impossible, to straighten fingers or grasp an item.
“
We envisage our solution being used by patients at home. It would be complementary to traditional rehab techniques Dr Joseph Galea, ImpHandRehab
‘These hand impairments can severely impact daily life,’ said Dr Joseph Galea, a researcher in motor neuroscience at the University of Birmingham in the UK.
‘Though there’s been a lot of focus on improving large, reaching-arm movements after a stroke, there’s been little work on improving hand functionality.’
Dr Galea wants to improve hand-movement recovery through the ImpHandRehab project. With funding from the European Research Council, this project asks stroke patients to perform tasks involving increasingly complex hand movements – a form of rehabilitation that will ultimately improve dexterity and quality of life. Users perform their tasks wearing a VR headset paired with affordable, off-the-shelf motion-capture gloves.
What motivates users to stick to their tasks?
Immersive VR
‘Gaming,’ explained Dr Galea. ‘We’ve developed two really immersive VR games that reward people for doing better and better at something like popping a balloon or controlling a submarine. We’ve noticed that the more points or coins are at stake, the harder a person will try and the better they’ll perform.’
Best of all, he and his colleagues have found that after a game has been played for a prolonged period of time, the improved hand performance persists even when the VR headset is removed.
‘We envisage our solution being used by patients at home,’ said Dr Galea.
‘It would be complementary to traditional rehab techniques.’
Watch the animation
Demonstration of VR training for stroke treatments. © Joseph Galea
Research in this article was funded via the EU’s European Research Council. If you liked this article, please consider sharing it on social media.